More Top Stories
Solar power battery repairs ‘could take up to 12 months’
15 April 2024
Police shortage leads to drop in checkpoints
9 April 2024
Sarakura declared new Penrhyn MP
16 March 2024
Govt says $1.3m invested in Lady Samoa charter
22 February 2024
Mass milkfish die-off in Penrhyn raises concerns
3 April 2024
Regulator defends Starlink users
9 April 2024
Aitutaki’s heritage preserved in new anthology
4 January 2024
Avatiu Eels retain Nines title
8 January 2024
Beddoes crowned top athlete
8 January 2024
NRL player Dargan dies in Aitutaki motorcycle crash
24 December 2023
‘Please heed the signs’: resident makes plea to tourists
20 December 2023
Cook Islands set to play in new World Series
10 October 2023
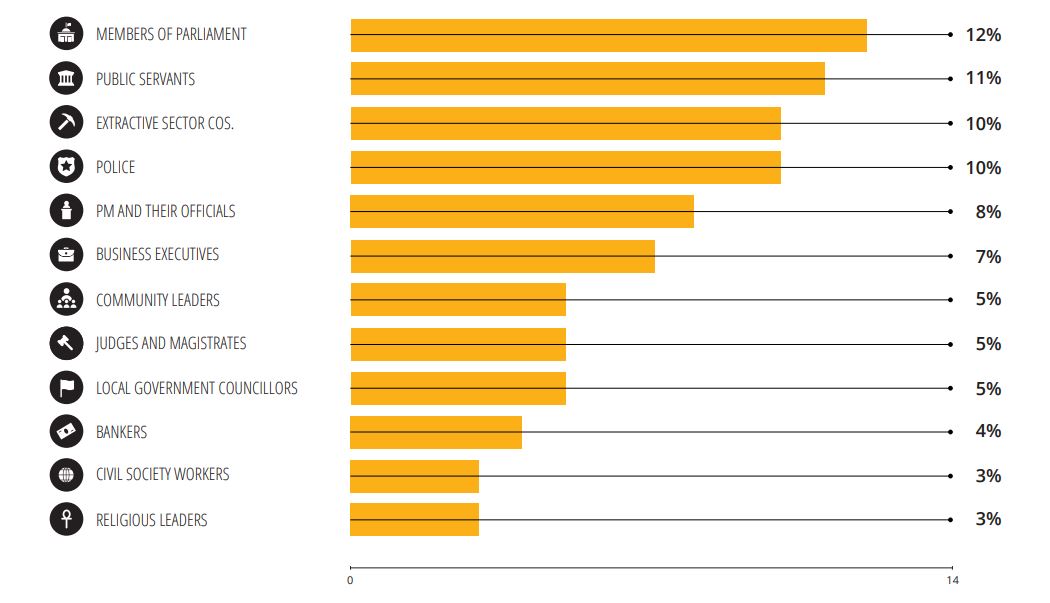
Corruption report exposes ‘bribe and sexual favours’
17 January 2023
Corruption in the Cook Islands?
21 January 2023
Moana target 2025 World Cup
11 November 2022
Mental health workshop answers many questions
Monday 22 October 2018 | Published in Virtues in Paradise
Share
Have you ever wondered what is the difference between mental illness and madness?
Have you ever wondered what is the difference between mental illness and madness?
To continue reading this article and to support our journalism
CLICK HERE TO SUBSCRIBE NOW
for as little as $11 per month.
- Up to date and breaking news
- Includes access to Premium content
- Videos and online classifieds
Already a subscriber, click here